CHARLOTTE, N.C. — Purple flags, representing the nearly 300 Mecklenburg County residents who died of opioid overdose in 2023, fluttered in the humid breeze last August in recognition of International Overdose Awareness Day on the city’s predominantly Black west side.
As recently as five years ago, the event might have attracted an overwhelmingly white crowd.
But the gathering on the last day of the month at the Valerie C. Woodard Community Resource Center drew large attendance from Black people eager to learn more about a crisis that now has them at the center.
In recent years, the rate of overdose deaths from opioids — originally dubbed “Hillbilly heroin” because of their almost exclusive misuse by white people — has grown significantly among Black people. This is largely due to the introduction of fentanyl, a synthetic opioid 50 to 100 times as powerful as morphine, which is often mixed into heroin and cocaine supplies and can be consumed unknowingly. In North Carolina, Black people died from an overdose at the rate of 38.5 per 100,000 residents in 2021 — more than double the rate in 2019, according to North Carolina Department of Health and Human Services data.
Terica Carter, founder of Hajee House Harm Reduction, a Charlotte-based nonprofit that co-organized the event with the county’s public health office, has been working to change that statistic. Seven years ago, she founded Hajee House after the overdose death of her 18-year-old son, Tahajee, who took an unprescribed dose of Percocet that he didn’t know was laced with fentanyl. Her nonprofit has since focused on addressing a critical issue in the fight against the opioid epidemic: that resources, treatment, and policy prescriptions have not followed the surge in addiction and overdoses among Black people.
“Nobody was acknowledging it, and I felt so alone,” Carter said. “That pushed me into not wanting anybody else to go through what I went through.”
Hajee House seeks to fill the gaps in resources and information about opioid overdose, substance use, and treatment. It also provides syringes, safe-use toolkits, the overdose reversal drug naloxone, fentanyl test strips, and recovery referral services — all in a familiar, neighborhood environment.
Despite efforts by groups like Hajee House, a lot of work remains in North Carolina. In 2019, for instance, white people accounted for 88% of those served by the opioid use prevention and treatment services funded by a $54 million grant from the federal Substance Abuse and Mental Health Services Administration, North Carolina Health News reported. Black people, meanwhile, made up about 24% of North Carolina’s population but only 7.5% of those served by the state assistance.
Nationally, Black people are half as likely as white people to be referred to or get treatment — even after a nonfatal overdose, according to the Centers for Disease Control and Prevention.
“If you are a Black person and have an opioid use disorder, you are likely to receive treatment five years later than if you’re a white person,” said Nora Volkow, director of the National Institute on Drug Abuse at the National Institutes of Health. “Five years can make the difference between being alive or not.”
According to the CDC, only 1 in 12 non-Hispanic Black people who died of an opioid overdose had been engaged in substance use treatment, while non-Hispanic white people had been treated at nearly twice the rate. Even those who seek care are less likely to complete the program and have poorer outcomes — which studies have linked to implicit bias and a lack of diversity and empathy for Black patients among treatment providers.

Daliah Heller, vice president of Drug Use Initiatives at Vital Strategies, a global health nonprofit, said she’s troubled by the lack of equal access to the full range of medications for opioid use disorder, which is considered the gold standard for care.
Those medications have the potential to reduce overdose risk by half and double a patient’s chances of entering long-term recovery. The FDA has approved three medications: buprenorphine and methadone, which are synthetic opioids that reduce cravings and withdrawal symptoms, and naltrexone, a post-detox monthly injectable that blocks the effects of opioids.
Black people are overwhelmingly treated with methadone. While methadone patients stay in treatment at higher rates compared with those prescribed buprenorphine, they face significant drawbacks, including difficulty finding a clinic, waitlists, and a requirement to visit the clinic every day to receive the medication under the supervision of a practitioner.
Meanwhile, buprenorphine can be prescribed in an office setting and filled at the pharmacy. A University of Michigan study found that white patients received buprenorphine three to four times as often as Black patients due to geographical availability and ability to pay.
“When buprenorphine came online in the early 2000s, we thought we could integrate that treatment alongside health care, and you wouldn’t need to go to a special program anymore,” Heller said. “That didn’t happen.”
Edwin Chapman, who runs an addiction clinic in Washington, D.C., said he must overcome many prescribing challenges to effectively treat his mostly Black patient population.
“The insurance companies in many states put more restrictions on patients in an urban setting, such as requiring prior authorization for addiction treatment,” Chapman said, speaking from his own experience working with patients. “The dosing standards were based on the white population and people who were addicted to pills. Our surviving Black population often needs a higher dose of buprenorphine.”
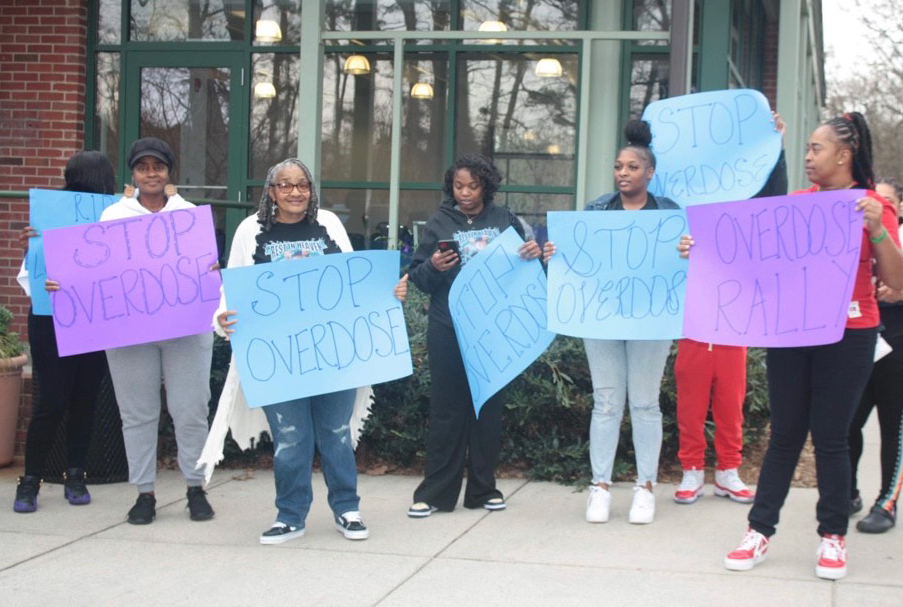
Heller said the lack of access to treatment is also driven by broader, systemic issues. She said many Black people fear that, by seeking social services, they might become ensnared in the criminal justice system and ultimately lose their employment, housing, or even custody of their children.
“Drug use occurs at the same levels across racial and ethnic groups, but Black Americans are more likely to be arrested and incarcerated on drug charges,” Heller said. “The more hyper-criminalized experience levied against Black communities interferes with access to care.”
All this is why there’s an increasing need for nonprofits like Hajee House that can provide information and a low-barrier access to services in the Black community, Carter said.
She credits the success of Hajee House to her personal connections and a keen understanding of the needs and cultural preferences of the Black community. When she holds overdose awareness events, for instance, she features cookouts, bouncy houses, and DJs to make them look more like block parties.
“We focus on making the events and outreach a comfortable, familiar environment for the Black community,” Carter said. “We’re Black, so we keep it Black.”
This article was produced by KFF Health News, a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF — the independent source for health policy research, polling, and journalism.
